Diabetes mellitus is a chronic condition that affects how the body regulates blood sugar (glucose). There are different types of diabetes, but the most common are Type 1 and Type 2 diabetes. While both result in high blood sugar levels, they differ in their causes, onset, management, and risk factors. Understanding these differences is essential for early diagnosis, proper treatment, and prevention of complications.
What is Type 1 Diabetes?
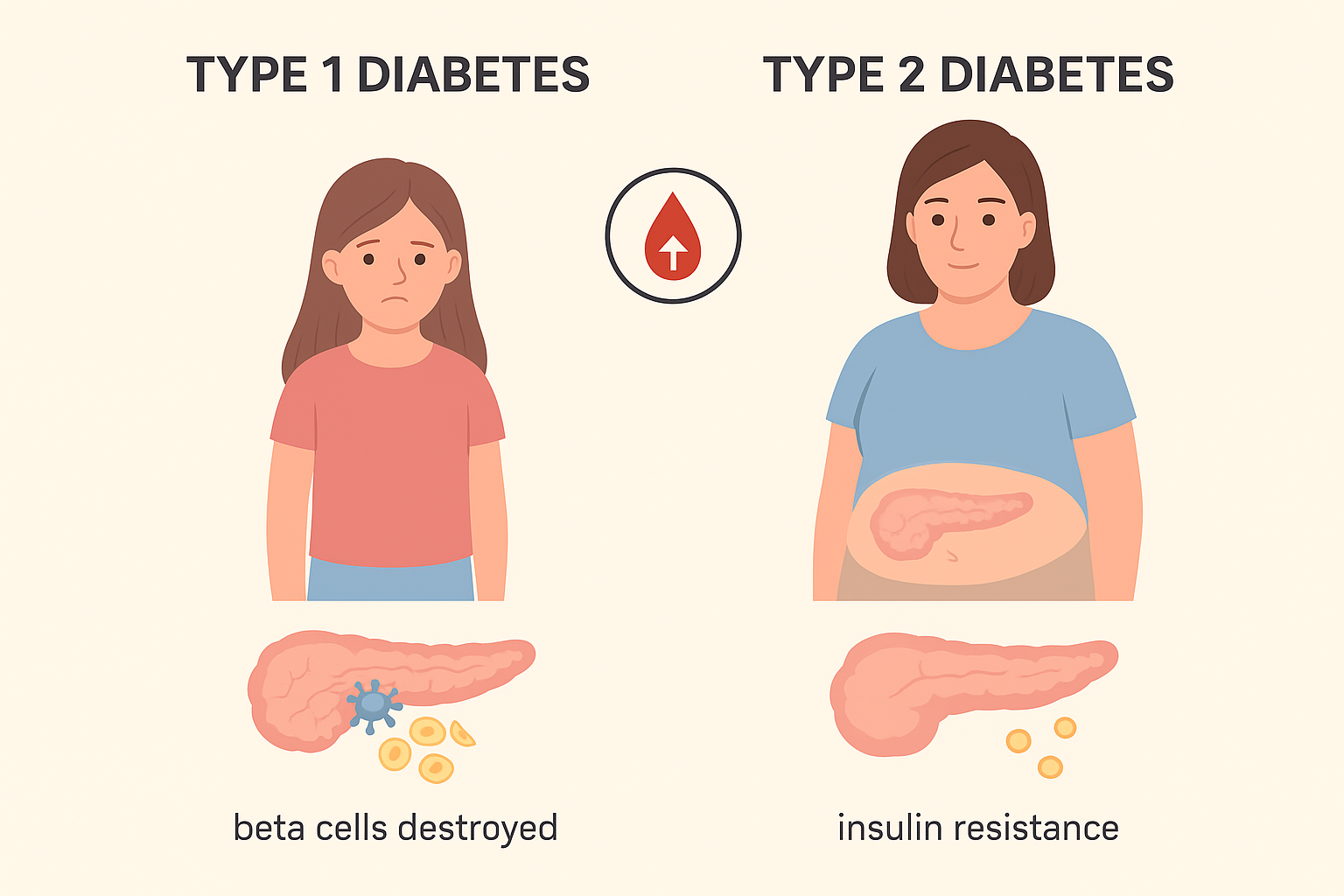
Type 1 diabetes is an autoimmune condition in which the body’s immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas. Without insulin, the body cannot move glucose from the bloodstream into the cells for energy.
- Onset: Usually occurs in childhood, adolescence, or early adulthood, but can develop at any age.
- Cause: Autoimmune reaction (exact cause is unknown).
- Insulin dependency: Patients must take insulin injections for survival.
- Prevalence: Less common, affecting about 5–10% of all diabetes cases.
What is Type 2 Diabetes?
Type 2 diabetes is a metabolic disorder where the body becomes resistant to insulin or does not produce enough of it. Unlike Type 1, insulin is still produced but not used effectively.
- Onset: Most commonly in adults over 40, but increasingly seen in children and young adults due to obesity and lifestyle changes.
- Cause: Combination of genetic factors, obesity, sedentary lifestyle, and poor diet.
- Insulin dependency: May be managed with lifestyle changes and medications, but some patients eventually need insulin.
- Prevalence: More common, accounting for about 90–95% of diabetes cases.
Key Differences Between Type 1 and Type 2 Diabetes
| Feature | Type 1 Diabetes | Type 2 Diabetes |
|---|---|---|
| Cause | Autoimmune destruction of insulin-producing cells | Insulin resistance + impaired insulin production |
| Onset Age | Childhood or adolescence (can occur in adults) | Usually adulthood, increasingly in younger people |
| Body Type | Often normal weight or underweight | Often overweight or obese |
| Insulin Production | Little to none | Reduced or ineffective |
| Treatment | Requires lifelong insulin therapy | Lifestyle changes, oral medicines, insulin if needed |
| Symptoms | Rapid onset: excessive thirst, frequent urination, weight loss, fatigue | Gradual onset: fatigue, slow wound healing, frequent infections, blurred vision |
| Prevention | Not preventable | Often preventable with healthy lifestyle |
Symptoms of Diabetes
Although Type 1 and Type 2 diabetes differ, some symptoms overlap:
- Excessive thirst (polydipsia)
- Frequent urination (polyuria)
- Unexplained weight changes
- Constant hunger
- Fatigue
- Blurred vision
- Slow healing of wounds
Type 1 symptoms appear suddenly, while Type 2 symptoms develop gradually over years.
Risk Factors
Type 1 Diabetes
- Family history of autoimmune diseases
- Genetic predisposition
- Viral infections (possible triggers)
Type 2 Diabetes
- Obesity and sedentary lifestyle
- Family history of type 2 diabetes
- Poor dietary habits (high sugar, refined carbs)
- Age above 40 years (though now common in younger people)
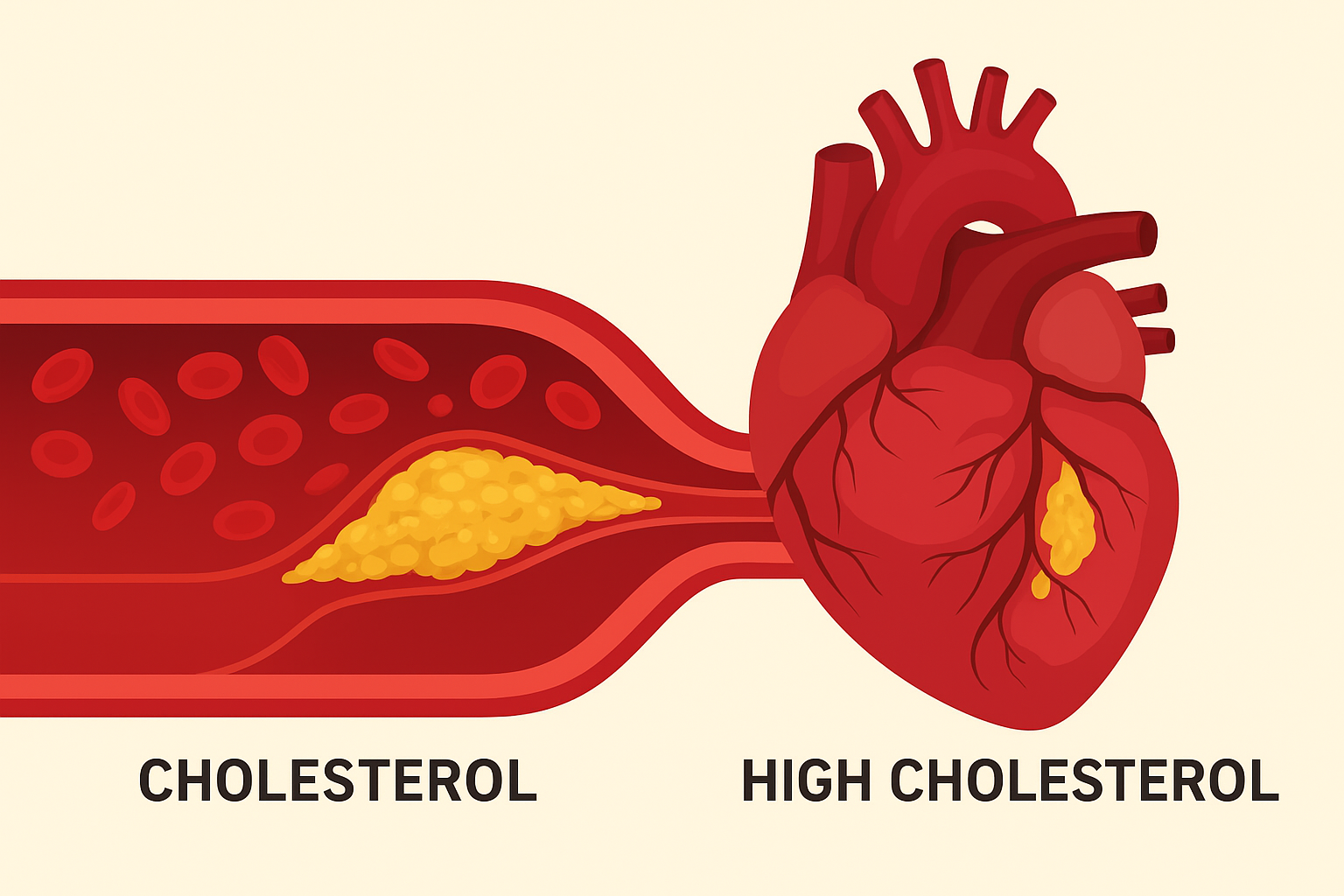
- High blood pressure and high cholesterol
Complications of Both Types
If untreated or poorly managed, both Type 1 and Type 2 diabetes can lead to serious complications such as:
- Heart disease and stroke
- Kidney disease (diabetic nephropathy)
- Nerve damage (neuropathy)
- Eye disease (retinopathy and blindness)
- Foot ulcers and amputations
Conclusion
Both Type 1 and Type 2 diabetes involve problems with insulin and blood sugar regulation, but their causes, onset, and treatments are very different. Type 1 is an autoimmune condition requiring lifelong insulin, while Type 2 is largely linked to lifestyle and can often be managed or even prevented with healthy changes.
Early detection, proper management, and lifestyle modifications can help people with diabetes live healthy, complication-free lives.