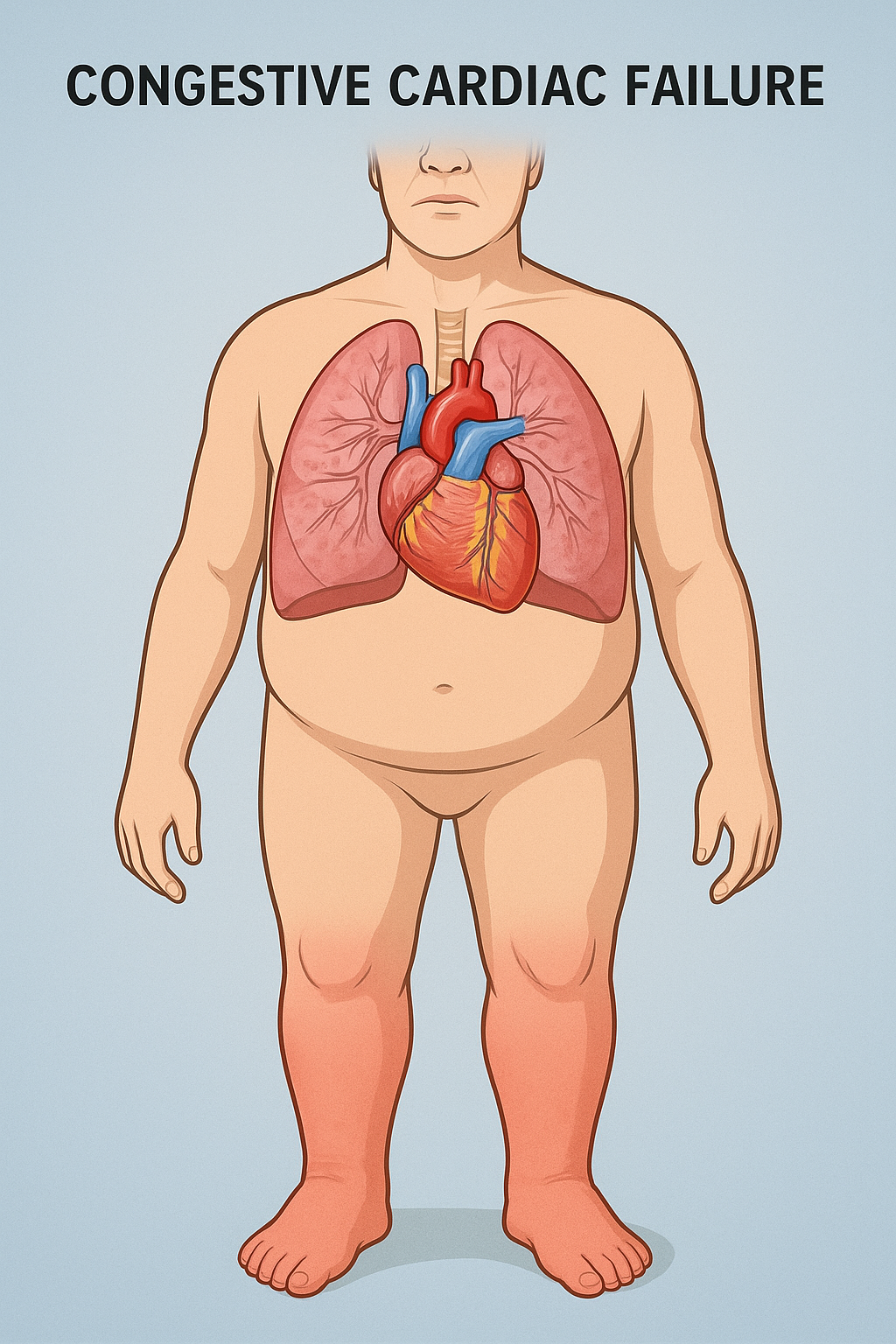
Congestive Cardiac Failure (CCF), commonly referred to as heart failure, is a chronic and progressive condition in which the heart muscle is unable to pump blood effectively to meet the body’s demands. As a result, blood and fluid build up in various parts of the body, leading to congestion—hence the term “congestive.”
This article provides a comprehensive overview of CCF, including its causes, risk factors, symptoms, diagnostic methods, and management options, in accordance with evidence-based medical guidelines.
What is Congestive Cardiac Failure?
CCF is not a disease itself but a clinical syndrome that arises due to structural or functional abnormalities of the heart. It can affect either the left ventricle, right ventricle, or both.
- Left-sided heart failure: Blood backs up into the lungs, causing breathlessness and pulmonary congestion.
- Right-sided heart failure: Blood pools in the veins, leading to swelling in the legs, ankles, and abdomen.
- Biventricular failure: When both sides of the heart are affected.
Causes and Risk Factors of CCF
Several conditions increase the likelihood of developing congestive cardiac failure:
- Coronary Artery Disease (CAD): Narrowing of coronary arteries reduces blood supply to the heart muscle.
- Hypertension (High Blood Pressure): Constant pressure overload makes the heart work harder.
- Valvular Heart Disease: Malfunctioning valves cause backflow or obstruction of blood.
- Cardiomyopathy: Weakening or stiffening of heart muscle due to genetic, metabolic, or infectious causes.
- Myocardial Infarction (Heart Attack): Damaged heart muscle reduces pumping efficiency.
- Diabetes Mellitus: Increases cardiovascular risk and worsens outcomes.
- Obesity and Sedentary Lifestyle.
- Alcohol abuse, smoking, and certain drugs.
Symptoms of Congestive Cardiac Failure
Patients with CCF may experience a wide range of symptoms depending on the severity and side of heart involvement:
- Shortness of breath (dyspnea) especially on exertion or when lying flat (orthopnea).
- Paroxysmal nocturnal dyspnea (PND): Waking up breathless at night.
- Fatigue and reduced exercise tolerance.
- Swelling of feet, ankles, or abdomen (edema, ascites).
- Persistent cough with frothy sputum.
- Palpitations or irregular heartbeat.
- Weight gain due to fluid retention.
- Loss of appetite and nausea in advanced cases.
Stages of Heart Failure (ACC/AHA Classification)
- Stage A: At high risk but no structural disease or symptoms.
- Stage B: Structural heart disease without symptoms.
- Stage C: Structural disease with current or past symptoms of heart failure.
- Stage D: Advanced disease requiring specialized interventions (e.g., heart transplant, mechanical support).
Diagnosis of Congestive Cardiac Failure
Diagnosis requires a combination of clinical evaluation, imaging, and laboratory tests:
- History and Physical Examination.
- Echocardiography (ECHO): Gold standard for evaluating ejection fraction (EF).
- Chest X-ray: May show cardiomegaly and pulmonary congestion.
- Electrocardiogram (ECG): Detects rhythm abnormalities or ischemia.
- Blood tests: BNP (B-type natriuretic peptide) or NT-proBNP are markers of heart failure.
- Cardiac MRI, stress test, or angiography in selected cases.
Management of Congestive Cardiac Failure
Treatment aims to improve symptoms, prevent progression, and reduce hospitalizations.
1. Lifestyle Modifications
- Salt restriction (low sodium diet).
- Fluid restriction in severe cases.
- Weight monitoring.
- Regular exercise and cardiac rehabilitation.
- Avoidance of alcohol and smoking.
2. Pharmacological Therapy
- ACE inhibitors or ARBs: Reduce afterload and improve survival.
- Beta-blockers: Improve heart function and reduce mortality.
- Diuretics: Relieve fluid overload.
- Aldosterone antagonists (spironolactone, eplerenone): Improve outcomes in advanced cases.
- ARNIs (sacubitril/valsartan): Newer agents showing significant benefits.
- Digitalis (Digoxin): In selected patients with persistent symptoms.
3. Device Therapy
- Implantable cardioverter-defibrillator (ICD): Prevents sudden cardiac death.
- Cardiac resynchronization therapy (CRT): For patients with conduction delays.
4. Advanced Interventions
- Left Ventricular Assist Devices (LVADs).
- Heart Transplant in end-stage cases.
Prognosis and Prevention
- Prognosis depends on age, severity, comorbidities, and adherence to therapy.
- Preventive measures include controlling hypertension, diabetes, obesity, and cholesterol, along with regular cardiac check-ups.
Conclusion
Congestive Cardiac Failure (CCF) is a serious but manageable condition. Early diagnosis, proper treatment, and lifestyle modifications significantly improve quality of life and survival. Raising awareness about risk factors, symptoms, and management strategies is essential for prevention and timely medical intervention.
If you experience symptoms suggestive of heart failure, consult a cardiologist promptly for evaluation and treatment.