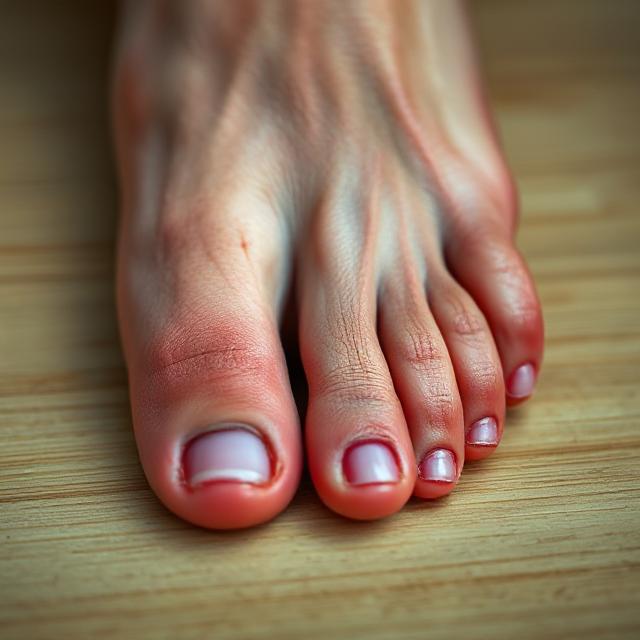
Nail candidiasis, also known as candidal onychomycosis, is a fungal infection of the nails caused primarily by Candida albicans. This condition is more common in individuals whose hands are frequently exposed to moisture or who have weakened immune systems. Nail candidiasis can cause pain, discoloration, and deformity of the nails, affecting both appearance and daily activities. Early recognition and proper management are essential to prevent complications and recurrence.
Causes of Nail Candidiasis
Nail candidiasis occurs when Candida species invade the nail bed or surrounding tissue. Several risk factors contribute to its development:
- Frequent Water Exposure: Dishwashing, laundry, or working in wet environments softens nails, making them more susceptible to infection.
- Diabetes Mellitus: High blood sugar supports fungal growth.
- Weakened Immune System: Conditions like HIV/AIDS, cancer, or long-term steroid use increase risk.
- Nail Trauma: Injury or aggressive manicures may damage the nail plate, allowing fungal entry.
- Use of Artificial Nails or Nail Polish: Traps moisture and encourages yeast growth.
- Prolonged Antibiotic Use: Disrupts normal skin flora, promoting Candida overgrowth.
Symptoms of Nail Candidiasis
The infection usually affects fingernails more than toenails and may show the following symptoms:
- Swelling and redness around the nail fold
- Pain or tenderness near the nail edges
- White, yellow, or brown discoloration of the nail
- Thickened, brittle, or distorted nail plate
- Separation of the nail from the nail bed (onycholysis)
- In severe cases, pus or fluid discharge from the nail fold
If left untreated, the infection can spread to other nails or surrounding skin.
Diagnosis
Diagnosis of nail candidiasis involves a combination of clinical examination and laboratory tests:
- Physical Examination: Observation of characteristic nail changes.
- Microscopy: A nail scraping examined under a microscope can reveal yeast cells or pseudohyphae.
- Fungal Culture: Confirms the Candida species and differentiates it from dermatophyte or bacterial infections.
Treatment Options
Treatment depends on the severity and extent of infection.
1. Topical Antifungal Treatments
- Antifungal creams or ointments containing clotrimazole, miconazole, or nystatin are applied to affected areas.
- Antifungal nail lacquers (e.g., ciclopirox or amorolfine) may help in mild cases.
2. Oral Antifungal Medications
- In moderate to severe infections, fluconazole, itraconazole, or ketoconazole may be prescribed for several weeks.
- Oral medications are usually more effective as the fungus can reside deep within the nail.
3. Nail Care and Hygiene
- Keep nails short, clean, and dry.
- Avoid prolonged exposure to water and irritants.
- Wear gloves when handling detergents or chemicals.
- Avoid sharing nail tools to prevent reinfection.
4. In Resistant Cases
- Partial or total nail removal may be considered if the infection is extensive or recurrent.
Prevention Tips
To reduce the risk of developing nail candidiasis:
- Keep hands and feet dry after washing.
- Avoid using harsh chemicals without gloves.
- Manage diabetes effectively.
- Maintain good nail hygiene and avoid trauma.
- Limit use of artificial nails and occlusive nail polish.
- Eat a balanced diet rich in vitamins and minerals to strengthen nails.
When to See a Doctor
Consult a healthcare professional if you experience:
- Persistent nail discoloration or thickening
- Pain, pus, or swelling around the nails
- Infection that does not improve with over-the-counter antifungals
- Multiple infected nails or signs of systemic illness
Conclusion
Nail candidiasis is a common but manageable fungal infection that can affect both nail health and appearance. With proper hygiene, early diagnosis, and effective antifungal treatment, most patients recover completely. Preventive care, particularly avoiding prolonged moisture and maintaining good hand hygiene, plays a key role in reducing recurrence.