Insulin resistance (IR) is a condition in which the body’s cells become less responsive to insulin — a hormone produced by the pancreas that helps glucose (sugar) enter the cells to produce energy. As a result, the pancreas produces more insulin to compensate. Over time, this can lead to high blood sugar levels, prediabetes, and eventually type 2 diabetes if left unmanaged.
Understanding insulin resistance is vital for preventing metabolic disorders and maintaining a healthy lifestyle.
What Is Insulin Resistance?
Under normal conditions, insulin binds to receptors on the surface of cells, allowing glucose to enter and be used for energy.
In insulin resistance, however, this process doesn’t work efficiently. The cells (especially in the liver, muscle, and fat) do not respond properly to insulin, resulting in elevated insulin and glucose levels in the bloodstream.
Causes of Insulin Resistance
There is no single cause of insulin resistance, but several factors contribute to its development:
- Genetic Factors: Family history of diabetes or metabolic disorders.
- Obesity: Particularly abdominal or visceral fat increases insulin resistance.
- Sedentary Lifestyle: Lack of regular physical activity reduces muscle glucose uptake.
- Unhealthy Diet: High intake of refined carbohydrates, sugary foods, and saturated fats.
- Hormonal Disorders: Conditions like polycystic ovary syndrome (PCOS) and Cushing’s syndrome.
- Chronic Stress: Elevated cortisol levels can affect insulin action.
- Sleep Disturbances: Poor sleep or sleep apnea can worsen insulin resistance.
Signs and Symptoms of Insulin Resistance
Insulin resistance often develops silently, but certain symptoms and signs may indicate its presence:
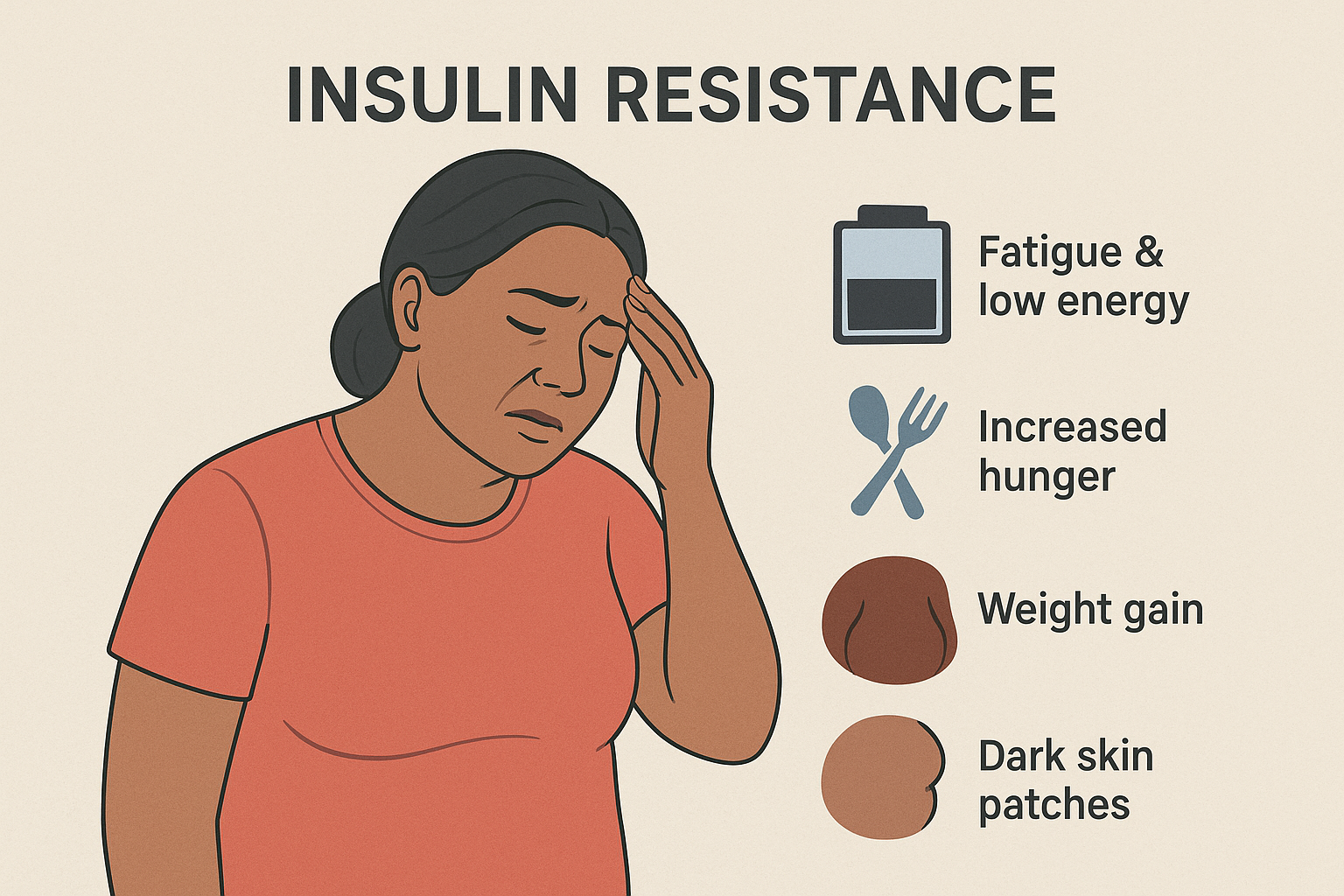
- Fatigue and low energy levels
- Increased hunger or sugar cravings
- Weight gain, especially around the abdomen
- Difficulty losing weight
- High blood pressure
- Dark, velvety skin patches (acanthosis nigricans) around the neck, armpits, or groin
- High triglycerides and low HDL cholesterol levels
Health Conditions Linked to Insulin Resistance
If left untreated, insulin resistance can lead to several metabolic and cardiovascular complications:
- Prediabetes and Type 2 Diabetes Mellitus (T2DM)
- Metabolic Syndrome
- Non-alcoholic fatty liver disease (NAFLD)
- Polycystic Ovary Syndrome (PCOS)
- Atherosclerosis and heart disease
- Hypertension (high blood pressure)
Diagnosis of Insulin Resistance
Insulin resistance is diagnosed using clinical tests that assess blood glucose and insulin function:
- Fasting Blood Glucose Test: Measures glucose after fasting for 8–10 hours.
- Oral Glucose Tolerance Test (OGTT): Evaluates glucose levels before and after consuming a glucose drink.
- HbA1c Test: Reflects average blood sugar levels over the past 2–3 months.
- Fasting Insulin Test: Measures insulin concentration in the blood.
- HOMA-IR (Homeostatic Model Assessment of Insulin Resistance):
- Calculated using fasting glucose and insulin values.
- A higher value suggests insulin resistance.
Management and Treatment of Insulin Resistance
There is no single medication to cure insulin resistance, but it can be effectively managed and even reversed with lifestyle modifications and medical supervision.
1. Healthy Diet
- Choose low-glycemic index (GI) foods such as whole grains, legumes, and vegetables.
- Avoid sugary drinks, refined carbs, and processed foods.
- Include lean proteins, healthy fats (olive oil, nuts, avocados), and fiber-rich foods.
- Practice portion control and balanced meal timing.
2. Regular Physical Activity
- Aim for at least 150 minutes of moderate-intensity exercise per week (walking, cycling, swimming).
- Add strength training to improve muscle insulin sensitivity.
3. Weight Management
- Even a 5–10% reduction in body weight can significantly improve insulin sensitivity.
4. Medications
- Metformin is commonly prescribed to improve insulin sensitivity in patients with prediabetes or type 2 diabetes.
- In some cases, GLP-1 receptor agonists or thiazolidinediones may be recommended.
5. Adequate Sleep and Stress Control
- Aim for 7–8 hours of quality sleep each night.
- Practice relaxation techniques such as yoga, meditation, or deep breathing.
Prevention of Insulin Resistance
Preventive measures include:
- Maintaining a healthy body weight
- Eating a balanced, whole-food diet
- Exercising regularly
- Managing stress and sleep
- Avoiding smoking and excessive alcohol intake
Conclusion
Insulin resistance is a reversible condition that plays a central role in the development of type 2 diabetes and other metabolic diseases. Early detection, lifestyle changes, and medical guidance are the key to preventing complications and maintaining long-term health.
By adopting healthy habits, individuals can significantly improve their insulin sensitivity, energy levels, and overall well-being.